- Clinical Study
- Changes in Glucose Metabolism after Adrenalectomy or Treatment with a Mineralocorticoid Receptor Antagonist for Primary Aldosteronism
-
Yu-Fang Lin, Kang-Yung Peng, Chia-Hui Chang, Ya-Hui Hu, Vin-Cent Wu, Shiu-Dong Chung, Taiwan Primary Aldosteronism Investigation (TAIPAI) Study Group
-
Endocrinol Metab. 2020;35(4):838-846. Published online December 2, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.797
-
-
5,163
View
-
131
Download
-
7
Web of Science
-
8
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Data on the effects of excess aldosterone on glucose metabolism are inconsistent. This study compared the changes in glucose metabolism in patients with primary aldosteronism (PA) after adrenalectomy or treatment with a mineralocorticoid receptor antagonist (MRA).
Methods
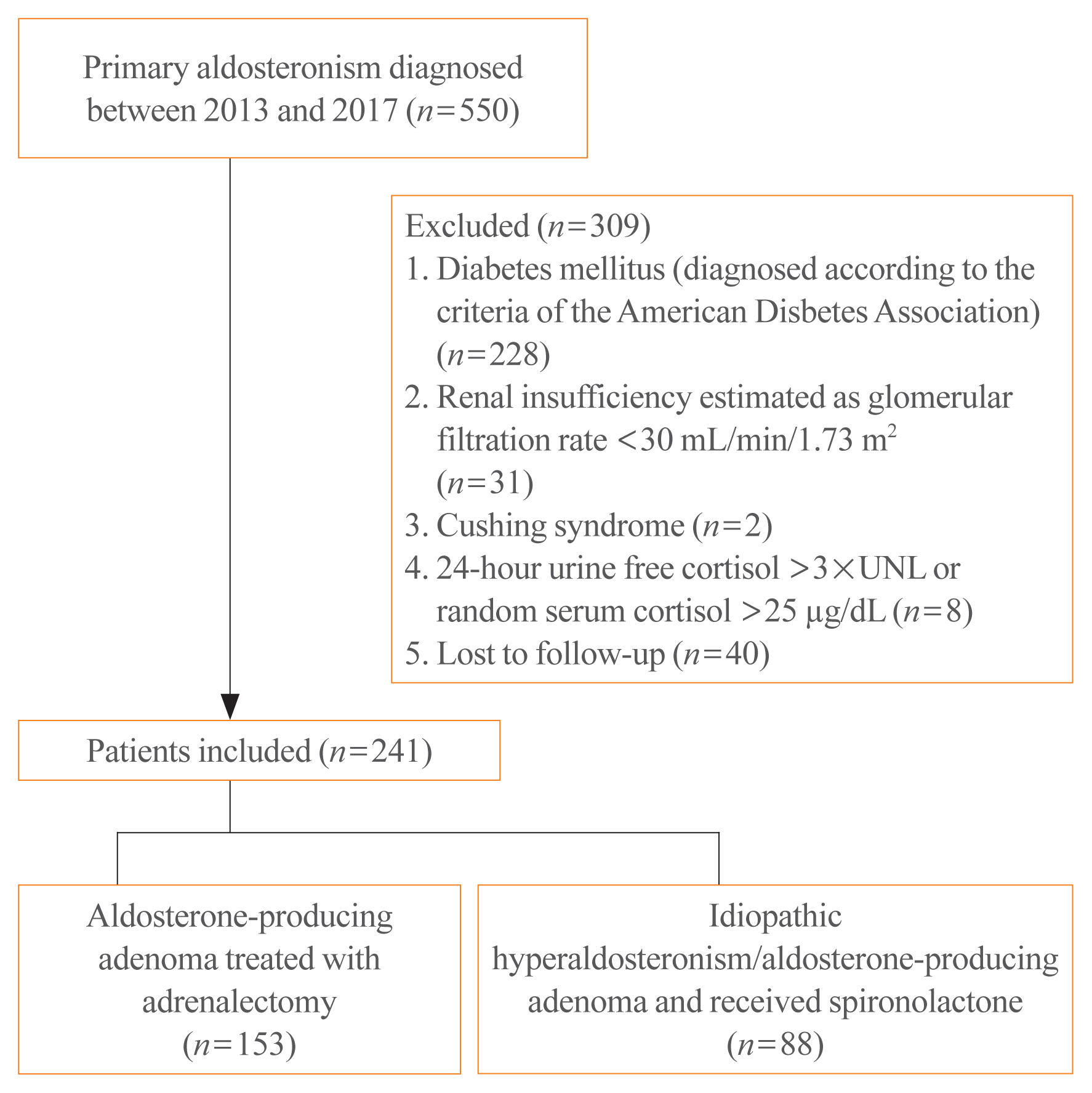
Overall, 241 patients were enrolled; 153 underwent adrenalectomy and 88 received an MRA. Fasting glucose, homeostatic model assessment of insulin resistance (HOMA-IR), and homeostatic model assessment of β-cell function (HOMA-β) were compared between the treatment groups after 1 year. Plasma aldosterone concentration (PAC) and factors determining HOMA-IR and PAC were evaluated.
Results
No baseline differences were observed between the groups. Fasting insulin, HOMA-IR, and HOMA-β increased in both groups and there were no significant differences in fasting glucose following treatment. Multiple regression analysis showed associations between PAC and HOMA-IR (β=0.172, P=0.017) after treatment. Treatment with spironolactone was the only risk factor associated with PAC >30 ng/dL (odds ratio, 5.2; 95% confidence interval [CI], 2.7 to 10; P<0.001) and conferred a 2.48-fold risk of insulin resistance after 1 year compared with surgery (95% CI, 1.3 to 4.8; P=0.007).
Conclusion
Spironolactone treatment might increase insulin resistance in patients with PA. This strengthened the current recommendation that adrenalectomy is the preferred strategy for patient with positive lateralization test. Achieving a post-treatment PAC of <30 ng/dL for improved insulin sensitivity may be appropriate.
-
Citations
Citations to this article as recorded by  - How should anti-hypertensive medications be adjusted before screening for primary aldosteronism?
Jin-Ying Lu, Yi-Yao Chang, Ting-Wei Lee, Ming-Hsien Wu, Zheng-Wei Chen, Yen-Ta Huang, Tai-Shuan Lai, Leay Kiaw Er, Yen-Hung Lin, Vin-Cent Wu, Hao-Min Cheng, Hsien-Li Kao, Charles Jia-Yin Hou, Kwan-Dun Wu, Szu-Tah Chen, Feng-Hsuan Liu
Journal of the Formosan Medical Association.2024; 123: S91. CrossRef - Diabete e sindrome metabolica nel paziente con iperaldosteronismo primario
Stella Bernardi, Valerio Velardi, Federica De Luca, Giulia Zuolo, Veronica Calabrò, Riccardo Candido, Bruno Fabris
L'Endocrinologo.2024; 25(1): 48. CrossRef - Prevalence, risk factors and evolution of diabetes mellitus after treatment in primary aldosteronism. Results from the SPAIN-ALDO registry
M. Araujo-Castro, M. Paja Fano, B. Pla Peris, M. González Boillos, E. Pascual-Corrales, A. M. García Cano, P. Parra Ramírez, P. Martín Rojas-Marcos, J. G. Ruiz-Sanchez, A. Vicente Delgado, E. Gómez Hoyos, R. Ferreira, I. García Sanz, M. Recasens Sala, R.
Journal of Endocrinological Investigation.2023; 46(11): 2343. CrossRef - Estimated glomerular filtration rate-dip after medical target therapy associated with increased mortality and cardiovascular events in patients with primary aldosteronism
Jia-Yuh Sheu, Shuo-Meng Wang, Vin-Cent Wu, Kuo-How Huang, Chi-Shin Tseng, Yuan-Ju Lee, Yao-Chou Tsai, Yen-Hung Lin, Jeff S. Chueh
Journal of Hypertension.2023; 41(9): 1401. CrossRef - Risk of dementia in primary aldosteronism compared with essential hypertension: a nationwide cohort study
Namki Hong, Kyoung Jin Kim, Min Heui Yu, Seong Ho Jeong, Seunghyun Lee, Jung Soo Lim, Yumie Rhee
Alzheimer's Research & Therapy.2023;[Epub] CrossRef - Secondary diabetes mellitus due to primary aldosteronism
Melpomeni Moustaki, Stavroula A. Paschou, Eleni C. Vakali, Andromachi Vryonidou
Endocrine.2022; 79(1): 17. CrossRef - Serum Cystatin C Levels Could Predict Rapid Kidney Function Decline in A Community-Based Population
Wei-Ching Fang, Hsing-Yu Chen, Shao-Chi Chu, Po-Hsi Wang, Chin-Chan Lee, I-Wen Wu, Chiao-Yin Sun, Heng-Jung Hsu, Chun-Yu Chen, Yung-Chang Chen, Vin-Cent Wu, Heng-Chih Pan
Biomedicines.2022; 10(11): 2789. CrossRef - Recovery from diabetes mellitus in primary aldosteronism patients after adrenalectomy
Yu Liu, Lede Lin, Chi Yuan, Sikui Shen, Yin Tang, Zhihong Liu, Yuchun Zhu, Liang Zhou
BMC Endocrine Disorders.2022;[Epub] CrossRef
- Adrenal gland
- Primary Aldosteronism and Cerebrovascular Diseases
-
Zheng-Wei Chen, Chi-Sheng Hung, Vin-Cent Wu, Yen-Hung Lin
-
Endocrinol Metab. 2018;33(4):429-434. Published online November 30, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.4.429
-
-
4,894
View
-
67
Download
-
21
Web of Science
-
20
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
As diagnostic techniques have advanced, primary aldosteronism (PA) has emerged as the most common cause of secondary hypertension. The excess of aldosterone caused by PA resulted in not only cardiovascular complications, including coronary artery disease, myocardial infarction, arrhythmia, and heart failure, but also cerebrovascular complications, such as stroke and transient ischemic attack. Moreover, PA is associated more closely with these conditions than is essential hypertension. In this review, we present up-to-date findings on the association between PA and cerebrovascular diseases. -
Citations
Citations to this article as recorded by  - Association of Dip in eGFR With Clinical Outcomes in Unilateral Primary Aldosteronism Patients After Adrenalectomy
Jui-Yi Chen, Kuo-How Huang, Yen-Hung Lin, Jeff S Chueh, Hsien-Yi Wang, Vin-Cent Wu
The Journal of Clinical Endocrinology & Metabolism.2024; 109(3): e965. CrossRef - Aldosterone and aldosterone synthase inhibitors in cardiorenal disease
Subodh Verma, Avinash Pandey, Arjun K. Pandey, Javed Butler, John S. Lee, Hwee Teoh, C. David Mazer, Mikhail N. Kosiborod, Francesco Cosentino, Stefan D. Anker, Kim A. Connelly, Deepak L. Bhatt
American Journal of Physiology-Heart and Circulatory Physiology.2024; 326(3): H670. CrossRef - Cardiovascular and metabolic characters of KCNJ5 somatic mutations in primary aldosteronism
Yi-Yao Chang, Bo-Ching Lee, Zheng-Wei Chen, Cheng-Hsuan Tsai, Chin-Chen Chang, Che-Wei Liao, Chien-Ting Pan, Kang-Yung Peng, Chia-Hung Chou, Ching-Chu Lu, Vin-Cent Wu, Chi-Sheng Hung, Yen-Hung Lin
Frontiers in Endocrinology.2023;[Epub] CrossRef - Risk of dementia in primary aldosteronism compared with essential hypertension: a nationwide cohort study
Namki Hong, Kyoung Jin Kim, Min Heui Yu, Seong Ho Jeong, Seunghyun Lee, Jung Soo Lim, Yumie Rhee
Alzheimer's Research & Therapy.2023;[Epub] CrossRef - Study on the Association between Primary Aldosteronism and Cerebrovascular Disease
·阿卜杜克热木 阿依努尔
Advances in Clinical Medicine.2023; 13(10): 16819. CrossRef - Anticoagulant therapy in patients with atrial fibrillation and chronic kidney disease: Arguments for or against
A. G. Komarova, N. L. Lyakhova, S. D. Covantsev, E. A. Naryshkina, D. V. Slepukhova
Medical alphabet.2023; (25): 14. CrossRef - Hypertension outcomes of adrenalectomy for unilateral primary aldosteronism
Igor Hartmann, Frantisek Hruska, Jan Vaclavik, Eva Kocianova, Zdenek Frysak, Marika Nesvadbova, Zbynek Tudos, Filip Ctvrtlik, Klara Benesova
Endocrine.2022; 76(1): 142. CrossRef - Cerebro-Cardiovascular Risk, Target Organ Damage, and Treatment Outcomes in Primary Aldosteronism
Xiao Lin, Muhammad Hasnain Ehsan Ullah, Xiong Wu, Feng Xu, Su-Kang Shan, Li-Min Lei, Ling-Qing Yuan, Jun Liu
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Primary Aldosteronism More Prevalent in Patients With Cardioembolic Stroke and Atrial Fibrillation
Van Nguyen, Tian Ming Tu, Marlie Jane B. Mamauag, Jovan Lai, Seyed Ehsan Saffari, Tar Choon Aw, Lizhen Ong, Roger S. Y. Foo, Siang Chew Chai, Shaun Fones, Meifen Zhang, Troy H. Puar
Frontiers in Endocrinology.2022;[Epub] CrossRef - Implication of MR Activity in Posttreatment Arterial Stiffness Reversal in Patients With Primary Aldosteronism
Zheng-Wei Chen, Chien-Ting Pan, Che-Wei Liao, Cheng-Hsuan Tsai, Yi-Yao Chang, Chin-Chen Chang, Bo-Ching Lee, Yu-Wei Chiu, Wei-Chieh Huang, Shuo-Meng Wang, Ching-Chu Lu, Jeff S Chueh, Vin-Cent Wu, Chi-Sheng Hung, Yen-Hung Lin
The Journal of Clinical Endocrinology & Metabolism.2022;[Epub] CrossRef - Time-Dependent Risk of Atrial Fibrillation in Patients With Primary Aldosteronism After Medical or Surgical Treatment Initiation
Kyoung Jin Kim, Namki Hong, Min Heui Yu, Hokyou Lee, Seunghyun Lee, Jung Soo Lim, Yumie Rhee
Hypertension.2021; 77(6): 1964. CrossRef - Pearls & Oy-sters: Cerebral Microbleeds Caused by Adrenocortical Adenoma-Related Primary Aldosteronism
Sun Min Lee, Yong Jun Choi, Kihwang Lee, Hyeung Kyoo Kim, Jin-Sun Park, Yong Cheol Lim, Jang-Hee Kim, So Young Moon
Neurology.2021; 96(20): 960. CrossRef - Cellular Senescence in Human Aldosterone-Producing Adrenocortical Cells and Related Disorders
Jacopo Pieroni, Yuto Yamazaki, Xin Gao, Yuta Tezuka, Hiroko Ogata, Kei Omata, Yoshikiyo Ono, Ryo Morimoto, Yasuhiro Nakamura, Fumitoshi Satoh, Hironobu Sasano
Biomedicines.2021; 9(5): 567. CrossRef - Contralateral Suppression at Adrenal Venous Sampling Is Associated with Renal Impairment Following Adrenalectomy for Unilateral Primary Aldosteronism
Ye Seul Yang, Seung Hun Lee, Jung Hee Kim, Jee Hee Yoo, Jung Hyun Lee, Seo Young Lee, A Ram Hong, Dong-Hwa Lee, Jung-Min Koh, Jae Hyeon Kim, Sang Wan Kim
Endocrinology and Metabolism.2021; 36(4): 875. CrossRef - Aldosterone Inhibits In Vitro Myogenesis by Increasing Intracellular Oxidative Stress via Mineralocorticoid Receptor
Jin Young Lee, Da Ae Kim, Eunah Choi, Yun Sun Lee, So Jeong Park, Beom-Jun Kim
Endocrinology and Metabolism.2021; 36(4): 865. CrossRef - Heart-Ankle Pulse Wave Velocity Is Superior to Brachial-Ankle Pulse Wave Velocity in Detecting Aldosterone-Induced Arterial Stiffness
Zheng-Wei Chen, Chien-Ting Pan, Cheng-Hsuan Tsai, Yi-Yao Chang, Chin-Chen Chang, Bo-Ching Lee, Yu-Wei Chiu, Wei-Chieh Huang, Yu-Li Lin, Vin-Cent Wu, Chi-Sheng Hung, Che-Wei Liao, Yen-Hung Lin
Biomedicines.2021; 9(10): 1285. CrossRef - Effects of nimodipine combined with betahistine on CRP and other inflammatory cytokines and vascular endothelial function in patients with hypertensive cerebral vasospasm
Xuanwei Liu, Na’na Zhao, Kexue Zeng, Peng Xiao, Pengjie Sheng, Xun Luo, Yulong Wang
Clinical Hemorheology and Microcirculation.2020; 75(3): 279. CrossRef - Associations between primary aldosteronism and diabetes, poor bone health, and sleep apnea—what do we know so far?
Huai Heng Loh, Norlela Sukor
Journal of Human Hypertension.2020; 34(1): 5. CrossRef - Predicting factors related with uncured hypertension after retroperitoneal laparoscopic adrenalectomy for unilateral primary aldosteronism
WuYun BiLiGe, Chaoqi Wang, JiRiGaLa Bao, Dahai Yu, A Min, Zhi Hong, Xiangbao Chen, Min Wang, Dongmei Wang
Medicine.2019; 98(30): e16611. CrossRef - Surgical Approach to Endocrine Hypertension in Patients with Adrenal Disorders
Jessica Shank, Jason D. Prescott, Aarti Mathur
Endocrinology and Metabolism Clinics of North America.2019; 48(4): 875. CrossRef
- CTNNB1 Mutation in Aldosterone Producing Adenoma
-
Jian-Jhong Wang, Kang-Yung Peng, Vin-Cent Wu, Fen-Yu Tseng, Kwan-Dun Wu
-
Endocrinol Metab. 2017;32(3):332-338. Published online September 18, 2017
-
DOI: https://doi.org/10.3803/EnM.2017.32.3.332
-
-
4,780
View
-
57
Download
-
9
Web of Science
-
9
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
Discoveries of somatic mutations permit the recognition of subtypes of aldosterone-producing adenomas (APAs) with distinct clinical presentations and pathological features. Catenin β1 (CTNNB1) mutation in APAs has been recently described and discussed in the literature. However, significant knowledge gaps still remain regarding the prevalence, clinical characteristics, pathophysiology, and outcomes in APA patients harboring CTNNB1 mutations. Aberrant activation of the Wnt/β-catenin signaling pathway will further modulate tumorigenesis. We also discuss the recent knowledge of CTNNB1 mutation in adrenal adenomas. -
Citations
Citations to this article as recorded by  - CTNNB1 in neurodevelopmental disorders
Wenting Zhuang, Tong Ye, Wei Wang, Weihong Song, Tao Tan
Frontiers in Psychiatry.2023;[Epub] CrossRef - Aldosterone-Regulated Sodium Transport and Blood Pressure
Akaki Tsilosani, Chao Gao, Wenzheng Zhang
Frontiers in Physiology.2022;[Epub] CrossRef - Pathogenesis of Primary Aldosteronism: Impact on Clinical Outcome
Lucas S. Santana, Augusto G. Guimaraes, Madson Q. Almeida
Frontiers in Endocrinology.2022;[Epub] CrossRef - Molecular Mechanisms of Functional Adrenocortical Adenoma and Carcinoma: Genetic Characterization and Intracellular Signaling Pathway
Hiroki Shimada, Yuto Yamazaki, Akira Sugawara, Hironobu Sasano, Yasuhiro Nakamura
Biomedicines.2021; 9(8): 892. CrossRef - Somatic mutations of GNA11 and GNAQ in CTNNB1-mutant aldosterone-producing adenomas presenting in puberty, pregnancy or menopause
Junhua Zhou, Elena A. B. Azizan, Claudia P. Cabrera, Fabio L. Fernandes-Rosa, Sheerazed Boulkroun, Giulia Argentesi, Emily Cottrell, Laurence Amar, Xilin Wu, Sam O’Toole, Emily Goodchild, Alison Marker, Russell Senanayake, Sumedha Garg, Tobias Åkerström,
Nature Genetics.2021; 53(9): 1360. CrossRef - Beta-Catenin Causes Adrenal Hyperplasia by Blocking Zonal Transdifferentiation
Emanuele Pignatti, Sining Leng, Yixing Yuchi, Kleiton S. Borges, Nick A. Guagliardo, Manasvi S. Shah, Gerard Ruiz-Babot, Dulanjalee Kariyawasam, Makoto Mark Taketo, Ji Miao, Paula Q. Barrett, Diana L. Carlone, David T. Breault
Cell Reports.2020; 31(3): 107524. CrossRef - Genetics and pathophysiology of low-renin arterial hypertension
A. L. Markel
Vavilov Journal of Genetics and Breeding.2019; 22(8): 1000. CrossRef - Diagnostic approach to low‐renin hypertension
Silvia Monticone, Isabel Losano, Martina Tetti, Fabrizio Buffolo, Franco Veglio, Paolo Mulatero
Clinical Endocrinology.2018; 89(4): 385. CrossRef - Genetic Characterization of GnRH/LH-Responsive Primary Aldosteronism
Nadia Gagnon, Katia Y Cáceres-Gorriti, Gilles Corbeil, Nada El Ghoyareb, Natasha Ludwig, Mathieu Latour, André Lacroix, Isabelle Bourdeau
The Journal of Clinical Endocrinology & Metabolism.2018; 103(8): 2926. CrossRef
|